Here at Trumpet Behavioral Health, we know your child’s well-being is your top priority. But, we also know that in order to be the most effective parent you can be, you need your sleep! And, to get the most from their childhood, so does your kiddo. To help you achieve the sometimes lofty goal of getting enough sleep, we’ve laid out some tips and a plan to help even the most difficult sleeper settle in and get some quality snooze time.
First, let’s take a closer look at how many children have sleep issues. Trust us, it’s not an uncommon problem. You are not alone in your sleeplessness. We’ll also examine just how much sleep your child actually needs. It’s probably MORE than you might think.
Sleep problems affect 35-50% of young children.
Common sleep problems documented by parents include nighttime routine compliance, not falling asleep when put to bed, sleep interfering behaviors, night awakenings and early awakenings. The amount of sleep can have an impact on the child’s health, behavior and overall well-being. Sleep problems increase to 67%-73% for young children with developmental disorders like autism spectrum disorder.
How long should my child sleep?
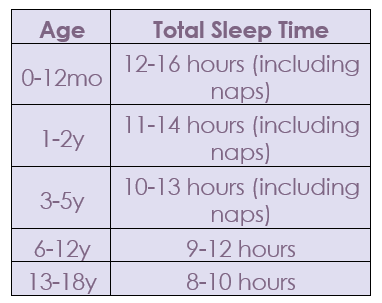
The amount of sleep on a regular basis your child should be getting should be based on chronological age. Averages come from the American Academy of Pediatrics to promote optimal health.
81% of children who see the pediatrician, psychiatrist or family physician for sleep problems result in a prescription for medication.
Behavior interventions have been shown to make significant improvements on sleeping behaviors in young children in 94% of documented studies. Some tried and true strategies are developing a positive nighttime routine, systematic approaches to night awakenings and bed time fading.
What is a Positive Nighttime Routine?
A series of activities, that occur approximately 30-40 minutes before you want your child to fall asleep or desired bedtime. These activities will prepare your child to “settle down”. When the series of activities are completed on a routine basis, they help indicate to the child’s body it is time to fall asleep.
How do I make a Positive Nighttime Routine?
- Identify 3-5 activities that your child enjoys (reading a book with you, coloring, etc.) PRO TIP: If any of your child’s activities include more movement than others, place the more physical activities at the beginning of your routine.
- Identify 2-3 activities that your child must do to get ready for bed (brush teeth, put on pajamas, etc. and add these into your routine). Avoid activities that may cause a tantrum. If cleaning up toys upsets your little one part of the time, keep it out of bedtime routine for now.
- Create a routine of your identified 5-7 total activities that you can keep the same every night at the same time. This is crucial!
- Avoid screen time in this routine (30-40 minute).
Don’t stress too much over your routine activities! Research tells us that it is more about the consistency of the routine and following through with the routine than the activities that make up the routine themselves. (Kodak and Piazza 2008)
How do I know my Positive Nighttime Routine is Effective?
Document or start a parent sleep diary to track your progress or identify patterns that may be helpful in improving your nighttime routine. Consider tracking things like:
- What time you bid your child goodnight and placed in bed.
- Time your child fell asleep.
- Final awake time at night.
- Number of nighttime awakenings.
- Total sleep duration.
- Number and duration of naps
Remember:
You CAN get through this.
We understand that when you’re tired, things don’t seem like they’ll ever improve. But, take heart. With a good bedtime routine, the whole family can get better sleep and everything will look brighter.

Christina Miller M.A., BCBA at Trumpet Behavioral Health in Cincinnati, OH
I earned my masters in Applied Behavior Analysis at Western Michigan University and have been working in the field of autism & other developmental disabilities for almost eight years. I have experience in severe problem behavior, early intervention & social skills. I am passionate about teaching others how Applied Behavior Analysis can have a positive impact on their daily life.
If you continue to have difficulties with bedtime, feeding, toileting and other challenging behavior during daily routines, call Trumpet Behavioral Health at 1-855-824-5669 to see if your child would benefit from behavioral services.
References:
American Academy of Pediatrics Supports Childhood Sleep Guidelines. (2016, June 13). Retrieved December 10, 2018
Delemere, E., & Dounavi, K. (2018). Parent-Implemented Bed Time Fading and Positive Routines for children with Autism Spectrum Disorders. Journal of Autism and Developmental Disorders,48, 1002-1019.
How much sleep do I need? (2017, March 02). Retrieved December 10, 2018
Jin, C., Hanley, G. P., & Beaulieu, L. (2013). An Individualized and Comprehensive Approach to Treating Sleep Problems In Young Children. Journal of Applied Behavior Analysis,46(1), spring 2013, 161-180.